Celebrating Congenital Diaphragmatic Hernia in April and Those Traveling to Tampa Bay for Care
April is Congenital Diaphragmatic Hernia Awareness Month.
Congenital Diaphragmatic Hernia (CDH) is a rare birth defect in which a hole in the diaphragm causes organs to migrate up, restricting lung growth. It is a life-threatening condition oftentimes diagnosed when a mother is pregnant and affects about one in every 3,000 babies. However, a specialty center in the Tampa Bay area is bringing families from all over the country for their child’s CDH care. The Center for Congenital Diaphragmatic Hernia at Johns Hopkins All Children’s Hospital, led by David Kays, M.D., was founded as the country’s first inpatient CDH unit with surgeons, nurses and other team members solely focused on CDH care.
At the 20-week anatomy scan, a mom may learn about her baby’s CDH diagnosis and may be told survival rates for the condition are around 50 percent. At Johns Hopkins All Children’s, well over 90 percent of babies with CDH survive, the highest in the nation. The CDH team is comprised of experts with extensive experience and unique treatment protocols that are executed with skilled precision. Through experience and more than two decades of research, Dr. Kays has developed a sense for timing the repair and managing the baby’s ventilation that provides the lungs and the brain the best chance to grow and develop.
“Doing the repair surgery does not make small lungs into big lungs,” Kays says. “Our goal is to allow small lungs to be as big as they can be.”
While CDH impacts the lungs, there can also be impacts to brain development.
“CDH leads to small lungs. Small lungs can lead to low oxygen levels,” Kays says. “We must deliver enough oxygen to the brain throughout the course of management to have good brain outcomes. We know that the number of kids we save is about how well we take care of their lungs. But we also know that the quality of that outcome—who they are when they go home—is all about how well we take care of their brain.”
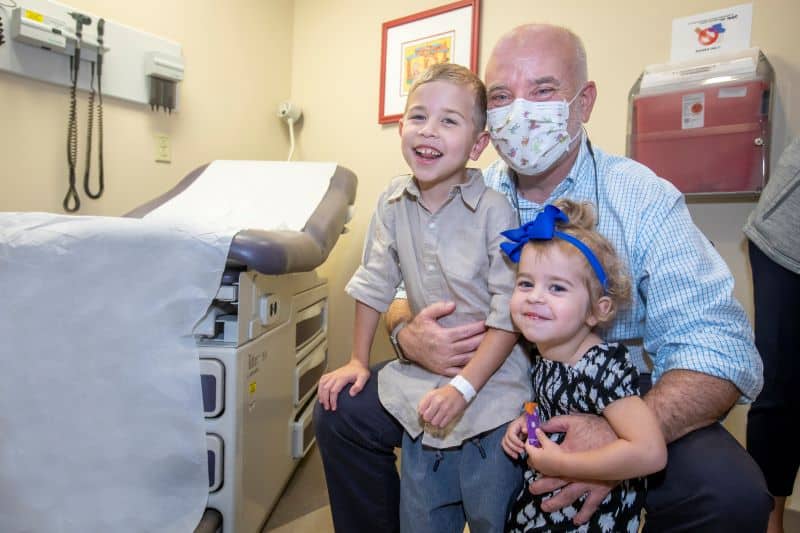
Kays adds that every baby treated at Johns Hopkins All Children’s gets a brain MRI and a neurodevelopmental test at discharge, including patients like Addy and Jaxson. Their cases are particularly rare — Jaxson was born first and needed the most aggressive form of life support, a heart-lung bypass called extracorporeal membrane oxygenation (ECMO) and a feeding tube. When Jaxson was 12 months old, Ally and Jimmy were surprised to learn they had another baby on the way, a happy, healthy baby girl, who is now 5. Then 2½ years later came another baby girl named Adelyn — “Addy.” But when it was time for her anatomy sonogram, it was like “being hit by lightning twice” for Ally and Jimmy. Addy also had CDH.
“It was extremely shocking. We definitely did not expect that. But Dr. Kays called us right away and it’s reassuring to know the capable hands that are going to be taking care of your baby and that there is a team that lives and breathes CDH,” Ally says.
While the two siblings had different experiences through their CDH journey, they still share a special bond, and most importantly, are doing great thanks to Kays and the team at Johns Hopkins All Children’s.
“Anytime that we see the team for follow-ups, it's very emotional because you get so close to them that they feel like family,” Ally says. “It’s a hard roller coaster to go through, but it’s worth it in the end. I would not trade Adelyn (or Jaxson) for anything in the world.”
BIO: Dr. Kays is the medical director of the Center for Congenital Diaphragmatic Hernia (CDH) at Johns Hopkins All Children’s and leads the first unit in the country exclusively dedicated to these patients. He also serves as director of the extracorporeal membrane oxygenation (ECMO) program and co-director of the Fetal Diagnosis/Treatment program. He joined the medical staff in 2016.
*Presented by Johns Hopkins All Children's Hospital